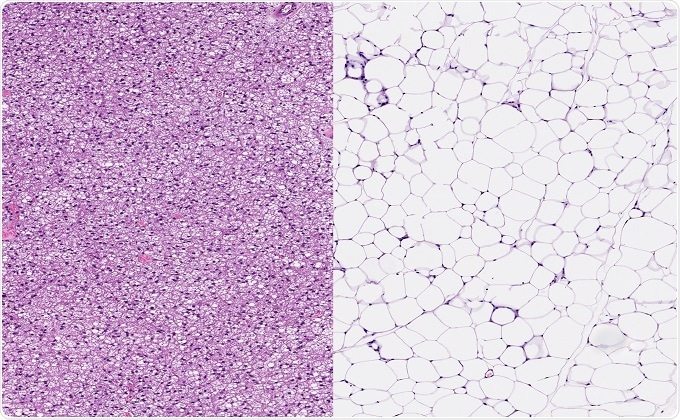
New Research Reveals Loss Of Smell Associated With Weight Loss In Mice
Research conducted at the University of California, Berkeley, suggest that the odor of food has a direct link with weight loss and how the body processes the calories. The new [...]